Introduction:
As an 18 -year TBI survivor, I have had my challenges with balance. Brain injury is known as the “invisible injury”, but I believe your ability to get your balance back is the one thing that reminds you that your injury is visible!
After my accident, I was in a wheelchair for about 6 months. While I was thankful to have the chair to get around, using a chair became limiting, and pushed my motivation to walk again!
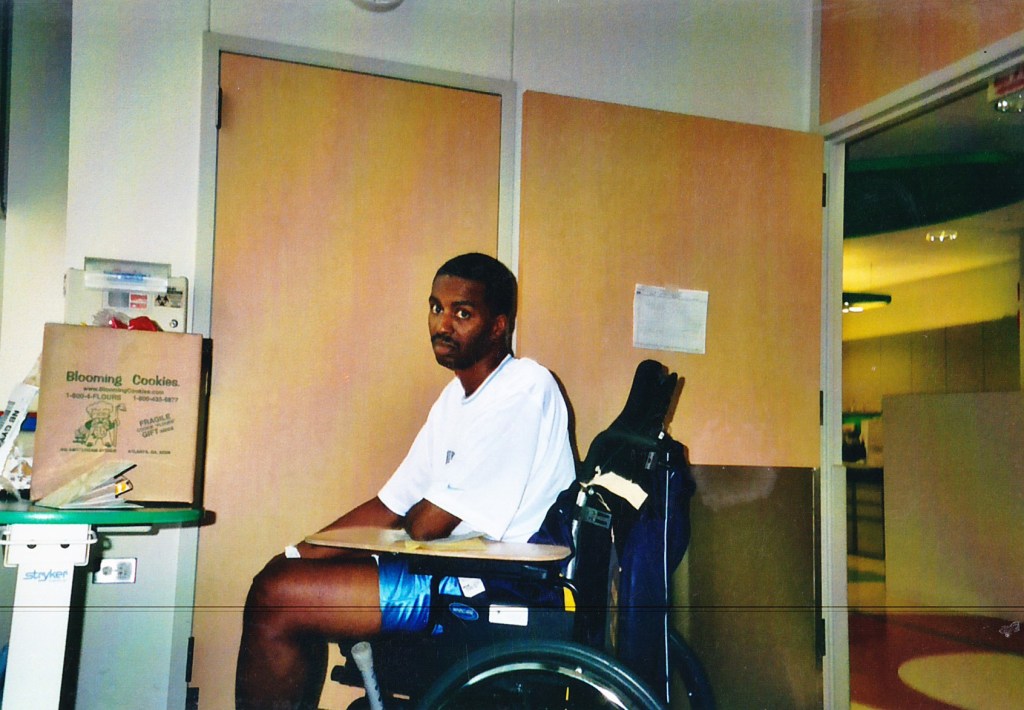
Now that I am 18 years post-accident, I believe I am in better shape, but I still struggle with balance issues.
I can run, but not very far, nor with the control I want.
Does that stop me from trying? No!
Will it stop me from challenging you to a race? No!
I clearly understand that I am not the athlete I was before the accident, and I know that I probably will not return to compete in the same way I had previously.
There are many things I can no longer do, but instead of focusing on those things, I am focusing on what I can do for others. And I am doing it with a smile!! I smile because it is a blessing to still be here, despite my injury. I believe I am making the most of this blessing called life, as I know am living on ‘gifted’ time! Thank you Lord!

Here is what I found on MSKTC.ORG on balance and everything related to it:
What is balance?
Balance is the ability to keep your body centered over your base of support. When standing, your base of support is your feet. When sitting, your base of support is your butt, thighs, and feet. Many factors affect your ability to keep your balance.
Falls are one of the main causes of TBI. Falls affect children (younger than 17) and older adults (older than 65) the most. Improving balance can help prevent TBIs.
If you have poor balance after a TBI, you have a high risk of falling. Falls can cause another TBI or a broken bone. Keeping your balance while sitting and standing is important for doing daily activities. These activities include walking and self-care tasks like bathing, using the toilet, and dressing. Poor balance can keep you from being able to play sports, drive, or work.
How quickly can your balance improve?
The extent of your injury and your health status before your injury determine how quickly
your balance problems will get better. Some balance problems can be treated effectively in one or two treatment sessions; others can take weeks, months, or years.
Research shows that:
- Most people with a TBI can walk on their own within 3 months of their injury. While most people walk again, many have problems moving quickly. They do not have the balance they need to return to activities such as running or sports.
With hard work, people with TBI can continue to improve their balance for many years after injury. But balance problems are more common in people with TBI than in people without TBI.
How can you improve your balance?
- Be cautious when working on your balance. Make sure you work at the right level to avoid falling when no one is around. A PT or OT can help design a program that is safe for you to practice at home.
- Increase your strength and flexibility. You can do stretches for your ankle and hip muscles. Other exercises will help strengthen your legs. These include mini squats, toe raises, or standing leg lifts. Go to www.nia.nih.gov/Go4Life for more information about these exercises. You can also talk to your doctor or PT about what you can do.
- Find your limits in balance. You can do this by moving your body over your feet as far as you can without lifting your feet. This will help you develop strategies to keep from losing your balance. You can also practice movements that allow you to move from one position to another. These movements include going from sitting to standing, reaching above your head to get something off a shelf, or picking up something on the ground.
- Practice standing or walking in different conditions. Practice standing with your eyes closed. This will decrease your dependence on using your vision for balance. Stand on a pillow; this will improve your ability to use your vision for balance. Change how far apart your feet are; bring them closer together or in front of one another. You can also stand on one leg.
- Practice activities that will improve your balance while walking. These include walking longer distances; walking and keeping up with someone else while talking; walking over different surfaces, such as on grass and sidewalks; and walking in crowded places such as the grocery store.
- Try a balance program that is based on evidence and designed for groups. Examples include A Matter of Balance, or the Otago Exercise Program. These programs may be available in your community.
Several of your body’s systems are involved in keeping your balance. Many health care providers diagnose and treat balance problems. These may include doctors who focus on physical medicine or rehabilitation (physiatrists) or doctors who focus on the nervous system and brain (neurologists). Other providers may include doctors who
focus on the ears, nose, and throat (otolaryngologists) and physical therapists (PTs). Your doctor may start by looking at the medicines you take. Medicines are a common cause of balance problems.
PTs and occupational therapists (OTs) use balance tests to identify specific problems and assess your risk for a fall. These tests also measure and track your progress with balance.
Treatment options
Balance problems have many different causes. Each cause requires a different treatment.
Your doctor, PT and OT, and other health care providers will work with you to find out and treat the different causes. Treatment needs to be tailored to your needs. It should also challenge you without compromising your safety.
Conclusion:
My issues related to balance usually occurred when I tried to multi-task, especially when walking. Early in my recovery, I was not able to successfully walk across a room while holding a glass full of water (not spilling) . However, after many failed attempts, I am better than I was years ago. I’ve also become better at successfully transporting objects that require both hands. Years ago, I would only attempt to walk while holding an object when I had one arm free. Back then, I needed one free arm so I could use it to balance myself walking, along with whatever I was carrying.
Adjusting to life after TBI has been a challenge, but for me, the road to getting better wasn’t about trying and failing. It was to keep trying until completion or until I was satisfied. I hated to fail before injury, and hate to fail now. If I tried to complete a task, and had some success at it, I’d kept trying, until I got it! I also learned that some things that I used to do are not as important to complete now. It is a matter of personal preference… I still would love to dominate on the basketball court and talk a little trash, but that isn’t important to me now. However, it’s a good to have pictures to remember my glory days! Let me give you an example of how expectations change:
Shortly after returning home from rehab, I used to get so upset with myself because I could no longer do what I wanted to do (driving, running, etc.). But, if I think about anyone that shares my experience, it’s important to be grateful what I can do or try today. Believe it or not, I get satisfaction from trying something new for the first-time post-accident! It’s my reminder to count my blessings!
Stay Strong Survivors!!

References
Katz, D. I., White, D. I., Alexander, M. P., & Klein, R. B. (2004). Recovery of ambulation after traumatic brain injury.
Archives of Physical Medicine and Rehabilitation, 85(6), 865–859.
McFayden, B. J., Cantin, J.-F., Swaine, B., Duchesneau, G., Doyon, J., Dumas, D., & Fait, P. (2009). Modalityspecific,
multitask locomotor deficits persist despite good recovery after a traumatic brain injury. Archives of
Physical Medicine and Rehabilitation, 90(9), 1596–1606.
Maskell, F., Chiarelli, P., & Isles, R. (2006). Dizziness after traumatic brain injury: overview and measurement in the
clinical setting. Brain Injury, 20(3), 293–305.
Patla, A. E., & Shumway-Cook, A. (1999). Dimensions of mobility: Defining the complexity and difficulty associated
with community mobility. Journal of Aging and Physical Activity, 7(1), 7–19.
Williams, G. P., & Schache, A. G. (2010). Evaluation of a conceptual framework for retraining high-level mobility
following traumatic brain injury: Two case reports. Journal of Head Trauma Rehabilitation, 25(3), 164–172.